Frontal Fibrosing Alopecia In Women: Early Signs And Management
Hair is deeply tied to identity, confidence, and self-expression for many women. So, when the hairline starts to thin or recede, it can feel frightening and confusing. One condition behind this change is frontal fibrosing alopecia (FFA)—an uncommon but increasingly recognized type of hair loss, especially among women over 40. FFA doesn’t just affect appearance; it can impact emotional well-being and social life. Understanding early signs, causes, and best ways to manage this condition is key to protecting hair health and confidence.
This article explores everything women should know about frontal fibrosing alopecia: how to spot early symptoms, what happens in your body, proven management options, and practical coping strategies. Whether you’re newly diagnosed, worried about your hairline, or supporting someone with FFA, this guide offers clear answers and practical advice.
What Is Frontal Fibrosing Alopecia?
Frontal fibrosing alopecia is a special type of scarring alopecia (also called cicatricial alopecia). It mainly affects the front and sides of the scalp. Hair follicles are gradually destroyed and replaced with scar tissue. Once lost, hair does not grow back in these areas.
The condition was first described in the early 1990s. Since then, reports have increased, especially in postmenopausal women. Experts aren’t sure if this rise is due to more awareness or an actual increase in cases. Some believe lifestyle changes and environmental exposures may play a part, while others think improved diagnosis is the main reason.
FFA is part of a group of hair disorders that cause permanent damage to follicles. Compared to other types of hair loss, FFA is unique for its pattern and the way it affects skin around the hairline. Many women notice that the affected areas feel different, often smoother or less oily, because the sweat and oil glands are damaged along with the follicles.
How Ffa Differs From Other Hair Loss
FFA is not the same as androgenetic alopecia (female pattern hair loss), which causes thinning but not scarring. In FFA, the hairline moves backward in a straight or band-like pattern, and the skin may look pale or shiny. Eyebrow and body hair can also be affected. Unlike some other types of alopecia, FFA is almost always permanent.
Other types of hair loss, like telogen effluvium, may cause sudden shedding but the hair usually grows back. Alopecia areata causes patchy, non-scarring loss, sometimes with regrowth. FFA’s “band-like” pattern is a strong clue—most women see a sharp, even edge where their hairline used to be, rather than a gradual thinning.
Who Is At Risk?
- Most common in women over 50, especially postmenopausal
- Can occur in women as young as their 30s
- Rarely affects men, but cases are reported
- More likely in those with a family history of autoimmune diseases
Women with lighter skin seem to be affected more, but FFA can occur in any ethnicity. A family history of autoimmune conditions, like thyroid disease or lupus, may increase risk. Some studies suggest that women who have used certain facial products regularly (like sunscreens or anti-aging creams) might be more prone, but the evidence is still weak.
Early Signs Of Frontal Fibrosing Alopecia
Recognizing FFA early makes a big difference in slowing down hair loss. Many women miss warning signs at first, thinking it’s normal aging or stress. Here are the earliest signals to watch for:
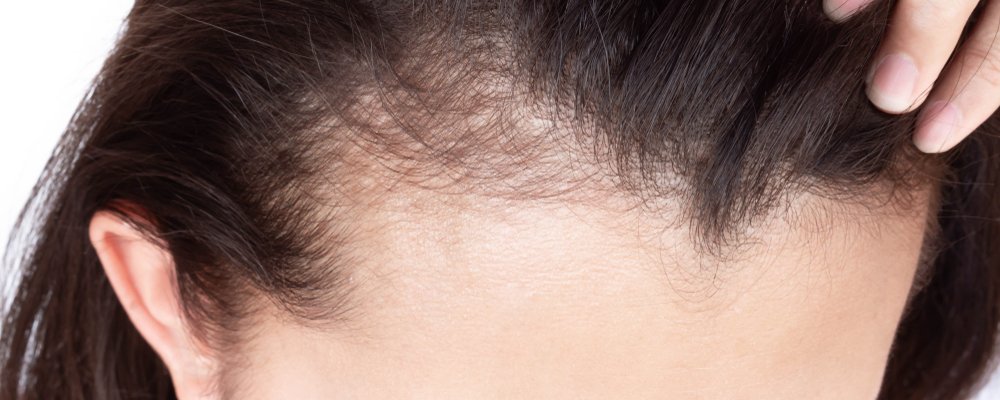
1. Receding Hairline
The classic sign is a slow, band-like hairline recession at the front or sides of the scalp. The hairline may look unnaturally “straight” or even, compared to normal aging which is more gradual and patchy. Sometimes, the recession is subtle—a few millimeters per year—but over time, it becomes obvious. Women may notice that their forehead appears larger or that their hair styling routine becomes more difficult.
2. Eyebrow Thinning
Up to 80% of women with FFA notice eyebrow loss—sometimes before scalp symptoms. The outer third of the eyebrows is often affected first. Some women lose all eyebrow hair. This can change facial expression and make makeup application challenging. Eyebrow thinning is often dismissed as aging or over-plucking, so it’s important to pay attention if this happens without any clear cause.
3. Itching, Burning, Or Redness
Early scalp symptoms can include a mild itchy or burning feeling, tenderness, or redness near the hairline. These symptoms may come and go. Sometimes, women feel a “tight” or prickly sensation when brushing or washing their hair. The skin may look slightly inflamed, and small bumps (follicular papules) can appear.
4. Fine “baby Hairs” Lost
The fine, soft vellus hairs at the very front of the scalp disappear. The skin here can look smoother or slightly lighter than the rest of the forehead. This loss is often noticed when women try to style their hair or apply makeup—the edge of the hairline feels “bare” or different.
5. Facial Or Body Hair Loss
Some women notice less hair on their arms, legs, or face (for example, sideburns or upper lip). This is less common but a significant clue. For example, the hair on the forearms may thin out, or the peach fuzz on the cheeks fades.
6. Scalp Changes
The affected skin may appear shiny, pale, or show tiny red bumps (follicular papules). There may be less sweating in these areas. Sometimes, the skin is more sensitive to sun or products.
Non-obvious Early Signs
- Loss of small facial “peach fuzz” hairs before scalp or eyebrow symptoms
- Difficulty applying makeup due to missing eyebrow “tail”
- Sunglasses or hats feeling looser because the forehead is higher
- The hairline feels “hard” or “fixed” compared to the rest of the scalp
Some women also notice that their hair part widens or that their hair is harder to style, especially if they used to wear it pulled back. These subtle changes often go unnoticed unless you are actively tracking your hairline.
Why Early Detection Is Hard
FFA progresses slowly and often without pain. Many women blame stress, diet, or menopause at first. Dermatologists say that many cases are only diagnosed after a year or more of symptoms.
Women often try to treat the problem themselves, using special shampoos, scalp massages, or supplements. Unfortunately, these rarely help with FFA, and the delay can lead to more permanent loss. Regular photos of your hairline and eyebrows can help catch changes that are easy to miss day-to-day.

Credit: mdsearchlight.com
Causes And Risk Factors
The exact cause of FFA is still unclear. But research highlights several key factors:
1. Autoimmune Reaction
FFA is considered a type of lichen planopilaris, an autoimmune disease. The body’s own immune system attacks hair follicles, causing inflammation and scarring. This immune attack is focused on the hair follicle’s stem cells, which are essential for hair growth. When these cells are destroyed, the follicle cannot regenerate.
2. Hormonal Changes
Most women develop FFA after menopause, suggesting hormones play a role. But younger women and men can also be affected. Estrogen levels drop after menopause, which may change the immune system or hair growth patterns.
3. Genetics
Some studies suggest a family history of autoimmune disease or certain genes increases risk. If your relatives have thyroid disease, lupus, or other autoimmune conditions, your risk may be higher.
4. Environmental Triggers
Recent research suggests that exposure to sunscreens or facial products may trigger FFA, but evidence is not conclusive. More studies are needed. Some dermatologists recommend avoiding certain products if you are at high risk, but this advice is not universal.
5. Other Possible Factors
- Smoking
- Chronic stress
- Thyroid problems
- Exposure to pollution or chemicals
Some dermatologists report that women who spend a lot of time outdoors or use many facial creams may develop FFA more often. However, no single factor explains all cases.
Non-obvious Insight
Some experts believe that rising FFA rates in women could be linked to changing lifestyle factors, such as increased use of skincare or anti-aging products, although this is still debated. It’s possible that new chemicals in cosmetics or changes in the environment are affecting immune responses in ways we don’t fully understand yet.
Another overlooked factor is chronic stress. While stress doesn’t cause FFA directly, it can affect immune function, possibly making the scalp more vulnerable.
How Ffa Progresses Over Time
FFA usually starts slowly. Without treatment, it can spread over several years. The recession may stop naturally in some women, but others see continued loss.
Typical Pattern
- Starts at the frontal hairline (forehead) or temples
- Moves backward 1-2 centimeters per year on average
- May affect the entire front of the scalp, sometimes ears to ears
- Eyebrow and body hair loss may begin before or after scalp symptoms
Women often report that their hairline changes shape, becoming straighter or more “masculine” in appearance. The loss is usually symmetric, but sometimes one side recedes faster.
Advanced Stages
- Loss of eyelashes or body hair
- Almost total destruction of hair follicles in affected areas
- No regrowth possible in scarred zones
- The scalp skin may feel “tight” or “waxy” in affected areas
Some women develop redness or bumps along the hairline, which can be itchy or tender. In the most severe cases, almost all frontal scalp hair, eyebrows, and even some eyelashes are lost.
How Fast Does It Progress?
Progression is different for each person. Some women lose hair quickly over months; others see slow change over many years. Factors like age, overall health, and early treatment can influence the rate.
Women who seek treatment early may slow progression, but there are no guarantees. In rare cases, the condition stabilizes after a few years, with no further loss. Most women, however, need ongoing management.
Insight
In rare cases, FFA may “burn out” after a few years, meaning the immune attack stops and hair loss stabilizes. However, lost hair almost never regrows. Recognizing “burnout” is hard—only a doctor can assess if your FFA is inactive.
Some women notice that stress, illness, or changes in medication can trigger periods of faster hair loss. This is why regular follow-up with a dermatologist is important.
Diagnosing Frontal Fibrosing Alopecia
Early and accurate diagnosis is essential for best results. Here’s how doctors confirm FFA:
1. Clinical Examination
A dermatologist looks for the classic band-like hairline recession, eyebrow loss, and skin changes. They may use a special magnifying glass (dermatoscope) to see miniaturized hairs or redness. The doctor checks for signs of scarring, such as loss of follicular openings (the tiny dots where hair grows).
Sometimes, the doctor will ask about family history, recent stress, or changes in medication, to rule out other causes.
2. Trichoscopy
This is a close-up scalp exam using a dermatoscope. It helps spot features like absent follicular openings, perifollicular erythema (redness), and scaling. Trichoscopy can show miniaturized hairs or areas where the skin is smooth and shiny—a sign of scarring.
In FFA, trichoscopy often reveals “perifollicular scale”—a white ring around follicles, and “follicular papules”—small bumps at the hairline.
3. Scalp Biopsy
A small piece of scalp skin is taken and examined under a microscope. This confirms scarring alopecia and rules out other causes. Biopsy shows inflammation around follicles and loss of stem cells—key for diagnosing FFA.
A biopsy is usually done with local anesthesia and leaves a tiny scar. It’s important for distinguishing FFA from other similar conditions.
4. Blood Tests
To check for autoimmune diseases, thyroid problems, or vitamin deficiencies, though most blood tests are normal in FFA. Blood tests may include thyroid function, ANA (autoimmune markers), vitamin D, and iron levels.
While blood tests rarely change treatment, they help rule out other hair loss causes.
How Ffa Is Different From Other Hair Loss
Many types of hair loss can look similar. Here’s a quick comparison:
| Feature | FFA | Female Pattern Hair Loss | Alopecia Areata |
|---|---|---|---|
| Hairline Recession | Yes, band-like | No, diffuse thinning | No, patchy loss |
| Eyebrow Loss | Common | Rare | Possible |
| Scarring | Yes | No | No |
| Inflammation | Often | Rare | Sometimes |
Key Insight
A scalp biopsy is the “gold standard” for diagnosis. Never start aggressive treatments without a clear diagnosis. Self-diagnosing FFA can lead to unnecessary treatments or missed underlying problems. If you see sudden patchy loss or widespread thinning, ask for a biopsy.
Management And Treatment Options
FFA can be challenging to treat, but early action can slow or stop progression. The main goals are to control inflammation, preserve remaining hair, and help patients cope.
1. Topical Treatments
- Corticosteroids: Powerful anti-inflammatory creams or gels, applied to the hairline or eyebrows. Often the first step. These help reduce redness, itching, and inflammation. Strong steroids can thin the skin if used too long, so doctors usually monitor usage.
- Calcineurin Inhibitors: Creams like tacrolimus or pimecrolimus reduce immune attack with fewer side effects than steroids. These are often used for eyebrow and facial areas where the skin is sensitive.
Sometimes, doctors combine these treatments, alternating steroids and calcineurin inhibitors to reduce side effects.
2. Oral Medications
- Antimalarials: Hydroxychloroquine is commonly used to calm immune activity. It’s usually given for 6-12 months, with regular eye checks for rare side effects.
- Tetracycline Antibiotics: Doxycycline or minocycline, which have anti-inflammatory effects. These help reduce redness and papules, but long-term use can cause stomach upset or sun sensitivity.
- 5-Alpha Reductase Inhibitors: Finasteride or dutasteride, usually for postmenopausal women, help by blocking hormones linked to hair loss. They are not recommended for women of childbearing age.
- Immunosuppressants: Drugs like methotrexate or mycophenolate for severe cases. These require careful monitoring and are reserved for aggressive or unresponsive FFA.
Combination therapy is common; doctors may use two or three medications to attack the problem from different angles.
3. Injections
- Steroid Injections: Given directly into the affected scalp to reduce inflammation quickly. Used for small areas or early cases. These can be very effective for eyebrow loss.
Injections are usually done every 4-6 weeks for a few months, then stopped if improvement is seen.
4. Light-based Therapies
- Low-Level Laser Therapy (LLLT): May help some women, but evidence is limited. LLLT is safe and painless but not proven for FFA. Some women use it as an add-on, hoping to stimulate remaining follicles.
5. Hair Transplantation
Not recommended unless the disease is inactive for several years, as transplanted hair can also be lost. Only for selected cases. Hair transplants are expensive and can fail if FFA is still active.
Women considering transplant should wait until FFA is stable for at least two years, with no new hairline recession.
6. Camouflage And Cosmetic Solutions
- Eyebrow pencils, powders, or tattoos: These help restore natural appearance and boost confidence. Microblading (semi-permanent tattooing) is popular but should be done by an experienced artist.
- Scalp micropigmentation: Creates the look of a fuller hairline using tiny dots of pigment.
- Hairpieces, wigs, or hair fibers: Modern wigs and fibers are light, comfortable, and look natural. Many women use these for special occasions or daily wear.
Cosmetic solutions don’t treat FFA but can be life-changing emotionally.
7. Lifestyle Changes
- Gentle hair care: Avoid tight styles, heat, or harsh chemicals. Choose soft brushes and mild shampoos.
- Sun protection: Wear hats; some experts suggest avoiding facial sunscreens until more evidence is available. If you do use sunscreen, choose mineral-based products and avoid applying them directly to the hairline.
- Stress management: Mindfulness or therapy for emotional support. Chronic stress affects immune health and can worsen symptoms.
Nutrition matters too. A balanced diet, rich in vitamins and minerals, supports hair and skin health.
Non-obvious Insights
- Early eyebrow tattooing can help some women adjust emotionally, even before scalp symptoms become severe. This can make the transition easier and restore self-esteem.
- Regular scalp photography (every 3-6 months) helps track progression and treatment effect. This is more accurate than memory and helps doctors make decisions.
Another insight: Some women find benefit from acupuncture or herbal supplements, but evidence is limited. Always discuss alternative treatments with your doctor.
What To Expect From Treatment
- Slowing or stopping further hairline recession is the main goal.
- Regrowth is rare, except possibly in eyebrows if treated very early.
- Most women need ongoing treatment for months to years.
- Side effects are possible, so regular doctor follow-up is important.
Managing expectations is key. FFA is a chronic condition, and even the best treatments may only stop progression. Emotional support and cosmetic solutions are just as important as medical therapy.
Credit: metrobostoncp.com
Comparing Treatment Effectiveness
Effectiveness depends on how early FFA is caught, age, and other health issues. Here’s a summary of common treatments:
| Treatment | Effectiveness (Stopping Loss) | Chance of Regrowth | Main Side Effects |
|---|---|---|---|
| Topical Steroids | Moderate | Low | Skin thinning |
| Hydroxychloroquine | Good | Very low | Eye effects (rare) |
| Finasteride/Dutasteride | Good | Very low | Hormone changes |
| Steroid Injections | Moderate | Low (eyebrows) | Pain, skin thinning |
Key Advice
Don’t expect a single “miracle cure. ” Most women need a combination of treatments and patience. Trying multiple approaches, under a doctor’s supervision, gives the best chance of slowing FFA.
Some women try supplements like biotin or vitamin D, but these rarely help if follicles are scarred. Focus on medical treatments and emotional support.
Living With Ffa: Emotional Support And Coping
Hair loss from FFA isn’t just physical. It can cause sadness, embarrassment, or anxiety. Here’s how to cope:
1. Get Educated
Understanding the condition helps reduce fear and confusion. Seek information from reliable sources and ask your doctor questions. Knowledge empowers you to make decisions and manage expectations.
2. Connect With Others
Support groups (online or in person) can help you feel less alone. Sharing experiences gives strength and practical ideas. Women in these groups often exchange tips for makeup, styling, and coping with social situations.
Some find comfort in knowing that FFA is not their fault and not caused by anything they did.
3. Consider Counseling
If hair loss is affecting your mood or self-esteem, a mental health professional can help you adjust. Therapy can teach coping skills, improve confidence, and help manage stress.
Social support is vital. Many women feel isolated or ashamed, but talking openly can lift some of that burden.
4. Explore Cosmetic Solutions
Many women find confidence through eyebrow makeup, wigs, or scalp camouflage. Experiment until you find what feels right. Cosmetic options can be empowering—don’t hesitate to try different products or techniques.
If you feel self-conscious, remember that many people use these solutions, even without hair loss.
5. Practice Self-care
Gentle hair care, healthy eating, and stress management all support overall well-being. Take time for activities you enjoy, and focus on strengths beyond appearance.
Non-obvious Coping Tips
- Try “before and after” photos to track progress and celebrate stability, not just regrowth. This helps you see the benefits of treatment, even if they are subtle.
- Involve family or close friends so they understand the emotional impact and can support you. Sharing your journey can reduce stress and build connection.
Another tip: Consider journaling your feelings about hair loss. Writing helps process emotions and clarify goals.
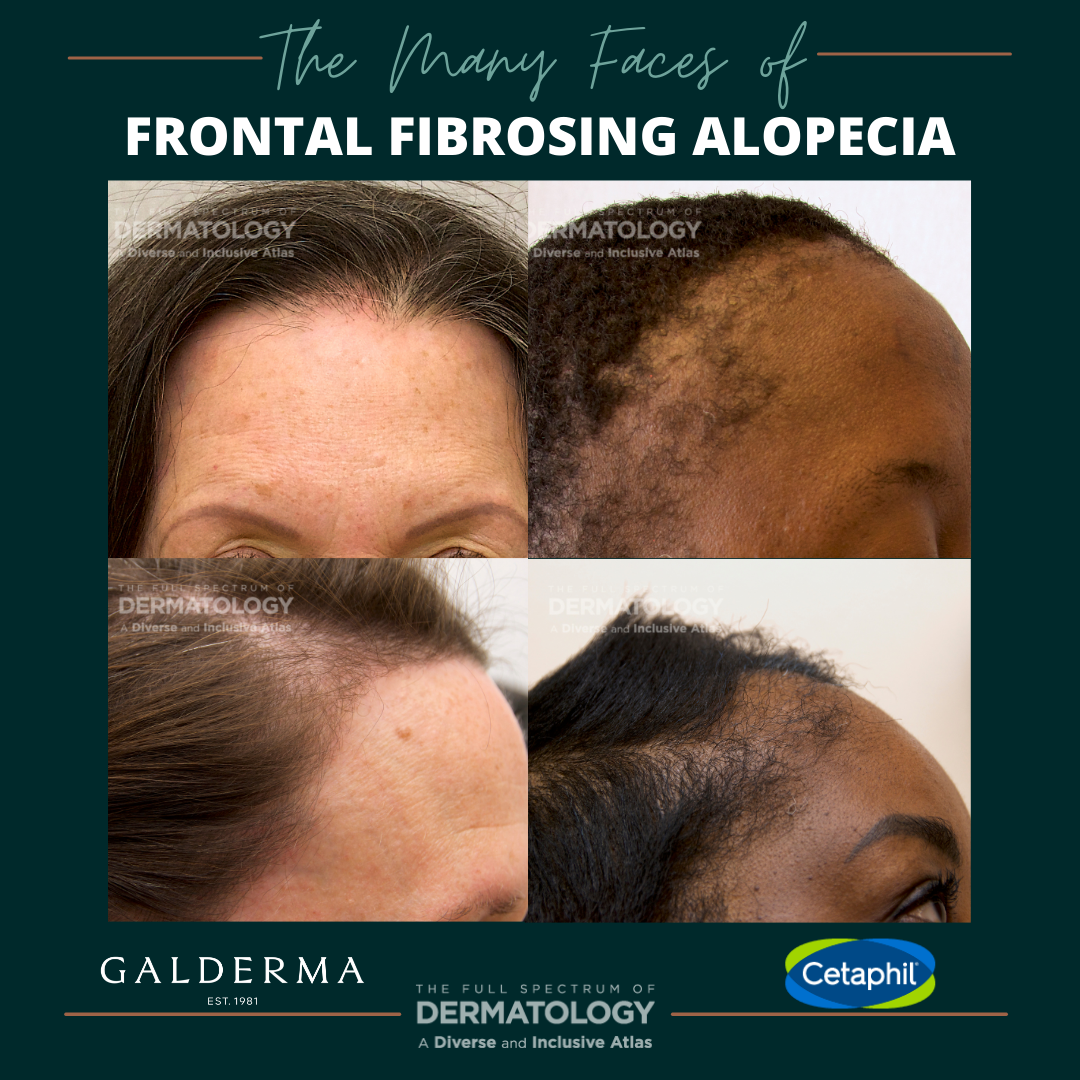
Credit: nextstepsinderm.com
Preventing Further Hair Loss
While there’s no guaranteed way to prevent FFA, you can take steps to reduce risk or slow progression.
1. Early Action
See a dermatologist quickly if you notice any early signs. The sooner treatment starts, the better the outcome. Don’t delay—waiting can mean more permanent loss.
2. Protect The Hairline
- Avoid tight hairstyles (braids, ponytails)
- Limit heat tools and chemical treatments
- Use mild shampoos and conditioners
Hair should be treated gently. Avoid brushing wet hair, and let it air dry when possible.
3. Sun And Skin Care
Use hats or scarves for sun protection. The link between sunscreens and FFA is unclear, so ask your doctor for advice on facial products.
If you use sunscreen, choose mineral-based types like zinc oxide, and avoid applying directly to the hairline. Consider using hats or umbrellas for extra protection.
4. Regular Check-ups
Follow up with your dermatologist every 3-6 months to monitor for changes. Regular exams help catch progression early and adjust treatment as needed.
Keep a diary of symptoms, treatments, and hairline changes. This helps your doctor tailor therapy.
5. Healthy Habits
No smoking, balanced diet, and stress reduction can support immune health. Smoking is linked to higher rates of scarring alopecia and can worsen FFA.
Stay active, sleep well, and manage stress. Mindfulness, yoga, or gentle exercise can help.
Insight
Many women focus only on the scalp, but eyebrow and body hair changes can be early warning signs. Act on these too. If you notice thinning in these areas, mention it to your doctor.
Another overlooked tip: Protect the scalp from harsh weather. Cold, wind, and pollution can irritate skin and worsen symptoms.
Research And Future Trends
FFA is an active area of research. Scientists are looking for new treatments and ways to predict who is at risk.
Promising Areas
- JAK inhibitors: New drugs that target immune pathways. Early studies in other hair loss types are encouraging. These medications may offer hope for FFA, but more research is needed.
- Genetic studies: Trying to find genes that increase FFA risk. If successful, this could lead to prevention or early detection.
- Environmental research: More focus on possible triggers like sunscreens, pollution, or cosmetics. Identifying real triggers could help with prevention.
Research is also exploring better ways to measure progression, like scalp imaging and blood markers.
What’s Still Unknown
- Why FFA rates are rising, especially in women
- Why eyebrows are affected first in many cases
- Why some women “burn out” and others continue to progress
Many experts are hopeful that new treatments will be found in the next decade. For now, early diagnosis and careful management are the best strategies.
For more on the latest research, see the National Institutes of Health.
Frequently Asked Questions
What Is The Difference Between Ffa And Lichen Planopilaris?
FFA is considered a clinical variant of lichen planopilaris (LPP). Both are scarring types of hair loss, but FFA mainly affects the frontal hairline and eyebrows, while LPP can impact any scalp area. The treatments are similar, but FFA has a more predictable pattern.
LPP may cause patchy loss anywhere on the scalp, and sometimes the skin is more itchy or painful than in FFA.
Is Ffa Contagious Or Caused By Poor Hygiene?
No. FFA is not contagious and has nothing to do with hygiene, diet, or washing frequency. It is an autoimmune process, not an infection.
FFA cannot be spread from person to person, and cleaning the scalp more often will not prevent it.
Can Hair Grow Back After Ffa?
Once hair follicles are destroyed and replaced with scar tissue, regrowth is not possible in those areas. Early treatment may help preserve hair and, in rare cases, allow some regrowth if follicles are only inflamed, not scarred.
Eyebrow regrowth is possible if treatment starts early. Scalp hair rarely returns unless the damage is minimal.
Does Ffa Affect Only Women?
FFA mainly affects postmenopausal women, but men and younger women can develop it too. The reasons for this gender difference are still being studied.
Some men develop FFA, usually with milder symptoms. Hormonal changes may explain why women are more affected.
Will Stopping Sunscreen Use Help Ffa?
Some studies suggest a link between frequent sunscreen use and FFA, but this is not proven. Do not stop using sun protection without talking to your dermatologist. Sunburn and skin cancer are also risks.
If you are concerned, ask your doctor about the safest sun protection for your skin and hairline.
Protecting your hairline is about more than appearance—it’s about self-confidence, identity, and feeling comfortable in your own skin. If you think you might have FFA, remember that early action gives you the best chance to slow or stop the process.
With good medical care, support, and coping strategies, women can manage FFA and continue to live fully and confidently.

