When you cut your finger or catch a cold, you might notice swelling, redness, or pain. These are clear signs of inflammation—your body’s natural defense when something is wrong. But inflammation is not always simple. It can protect you, but it can also damage your body’s barriers, like your skin or gut lining. This damage can trigger even more inflammation, leading to a cycle that is hard to break. Understanding how inflammation acts as a barrier damage trigger is key for good health, especially if you want to avoid chronic diseases, allergies, or autoimmune problems.
This article dives deep into how inflammation starts, how it damages barriers, and how this damage creates a vicious cycle. You will also learn practical ways to break this cycle and support your body’s natural defenses.
What Is Inflammation?
Inflammation is your body’s fast, smart way to protect itself. When you get hurt or face an infection, your immune system sends special cells to the problem area. These cells fight germs, clear debris, and help repair damage.
There are two main types of inflammation:
- Acute inflammation: This is short-term. It starts quickly and stops when the problem is fixed. For example, swelling after a sprained ankle.
- Chronic inflammation: This is long-lasting. It keeps going even when there’s no clear threat, often causing slow, hidden damage. Examples include arthritis, asthma, and inflammatory bowel disease.
Inflammation is not always bad. It helps you heal. But when it does not turn off at the right time, it can hurt your body’s barriers.
Inflammation also comes with other signs. You might feel heat in an area or even lose some function for a short time (like a stiff, swollen joint). These changes show your immune system is active. But if these signs last for weeks or months, it is a warning that your body is stuck in inflammation mode.
Sometimes, people do not even realize they have chronic inflammation. It can be silent, without pain or redness. Doctors often find it only after years, when damage has already happened. This is why paying attention to early symptoms and living a healthy lifestyle matters.
Understanding Body Barriers
Your body has several barriers that keep the inside safe from the outside world. The most important are:
- Skin
- Gut lining
- Lung lining (mucosa)
- Blood-brain barrier
These barriers work like tight walls. They stop germs, toxins, and harmful molecules from getting in. If these barriers are damaged, your body is open to more attacks.
Why Barriers Matter
Imagine your skin as a brick wall. Each cell is a brick, and sticky proteins act as mortar. If the wall breaks, germs get in more easily. The same idea applies inside your body. For example:
- The gut lining keeps bacteria in your gut from leaking into your blood.
- The lung lining stops dust, smoke, and germs from entering your body.
- The blood-brain barrier protects your brain from harmful chemicals.
Your eyes, mouth, and even the urinary tract have their own barriers. Each is designed for its environment. For example, your tears have special chemicals to kill bacteria before they enter through your eyes.
When these barriers are weak or broken, you can get sick more often. Weak barriers can also let in things that should not be there, like food particles or pollen, leading to allergic reactions or autoimmunity. Sometimes, your body even starts to attack itself, confusing your own cells for invaders.
A strong barrier system is the foundation of good health. That’s why skin care, gut health, and even breathing clean air are more important than many people think.
How Inflammation Damages Barriers
Inflammation should help your body heal, but sometimes, it does the opposite. Here’s how it can harm your barriers:
- Strong immune chemicals: Inflammation releases chemicals like cytokines and free radicals. These are meant to kill germs but can also hurt your own cells.
- Tight junction breakdown: Barriers like the gut have tight connections between cells. Inflammation can break these connections, making the barrier leaky.
- Cell death: If inflammation is too strong, it may kill cells that are needed to keep the barrier strong.
- Delayed repair: Chronic inflammation can slow down the repair process, so damage lasts longer.
When immune cells attack invaders, they release enzymes and acids that break down germs. But if these weapons are too strong or released for too long, they also eat away at the body’s own tissues. For example, in the gut, these chemicals can cause tiny holes, allowing harmful substances to slip through.
Example: The Leaky Gut
A common example is leaky gut. Normally, the gut lining is tight. But with inflammation, the wall gets holes. Bacteria and toxins slip through, causing more inflammation. This can lead to food allergies, autoimmune disease, and even brain fog.
Leaky gut does not only cause stomach problems. It can also affect your mood, energy, and immune system. When unwanted substances enter the blood, your body has to work harder to stay balanced. Over time, this may lead to problems like joint pain, skin rashes, or headaches.
Example: Eczema And Skin Barrier
People with eczema have inflamed, broken skin. The barrier is weak, so allergens and germs get in. This triggers more inflammation, more itching, and more damage—a never-ending cycle.
Even simple things, like soap or sweat, can trigger a flare-up in people with eczema. Their skin loses water more easily, so it gets dry and cracked. Scratching makes it worse and can let bacteria in, leading to infection.
The Inflammation-barrier Damage Cycle
When inflammation damages a barrier, the barrier becomes weak. This lets in more germs and toxins, which trigger even more inflammation. The cycle looks like this:
- Injury or trigger (like infection, stress, or chemicals)
- Inflammation starts to protect and repair
- Barrier damage (leaky gut, eczema, etc.)
- More invaders or irritants get in
- Even more inflammation happens
If this cycle keeps going, it can lead to chronic diseases.
This cycle can be hard to break once started. The longer it lasts, the harder it is for your body to heal. That is why early action is important.
How The Cycle Works In Different Barriers
Gut
A poor diet, alcohol, stress, or certain medicines can all trigger gut inflammation. This makes the gut lining leaky. Bacteria enter the blood, causing more inflammation and sometimes autoimmune disease.
For example, eating a lot of sugar or processed foods feeds bad bacteria, which make chemicals that harm the gut wall. People who take many antibiotics may lose good bacteria, making the gut even more open to damage.
Skin
Harsh soaps, dry air, or allergies can trigger skin inflammation. The damaged skin lets in irritants, causing eczema or infections.
Some people notice their skin barrier gets worse in cold, dry weather. Others react to new skin creams or detergents. Infections like athlete’s foot also happen more easily on broken skin.
Lungs
Air pollution or infections can cause lung inflammation. Damaged lung lining lets in more pollutants, leading to asthma or chronic bronchitis.
For example, people who live in cities with high pollution often have more lung problems. Even short-term exposure to smoke or fumes can start inflammation, especially if you have allergies.
Brain
If the blood-brain barrier is damaged by inflammation (as in some viral infections), toxins can enter the brain. This may raise the risk for conditions like multiple sclerosis or Alzheimer’s disease.
Some studies show that inflammation in the body, such as from gum disease or obesity, can also weaken the blood-brain barrier over time. This is why taking care of your whole body is important for your brain too.
Why Breaking The Cycle Matters
If the inflammation-barrier cycle continues, you may develop:
- Chronic diseases (arthritis, diabetes, heart disease)
- Autoimmune problems (like Crohn’s disease, lupus)
- Allergies and asthma
- Skin problems (eczema, psoriasis)
- Mental issues (anxiety, depression, brain fog)
Breaking the cycle is key to better health and long life.
When the cycle is broken, the body can heal. Inflammation goes down, barriers get stronger, and symptoms improve. This not only prevents disease but also improves quality of life—better energy, clearer thinking, and fewer infections.
Many people do not realize their fatigue, joint pain, or headaches are linked to ongoing barrier damage and inflammation. Seeing the connection can be the first step toward real change.
Common Triggers That Start The Cycle
Not everyone gets stuck in this cycle. Some triggers make it more likely:
- Infections: Viruses, bacteria, or parasites can start inflammation.
- Food choices: High sugar, processed foods, and alcohol cause more gut inflammation.
- Stress: Chronic stress increases inflammation and weakens barriers.
- Chemicals: Pollution, smoke, and harsh cleaning products damage skin and lung barriers.
- Allergens: Dust, pollen, and certain foods trigger immune responses.
- Medications: Some painkillers and antibiotics harm the gut lining.
- Genetics: Some people inherit weak barriers or overactive immune systems.
Some triggers are easy to control, like diet or exposure to chemicals. Others, like genetics, are not. But knowing your own risks can help you take action early. For example, if you have a family history of allergies or autoimmune disease, you might focus more on gut health and reducing stress.
Non-obvious Insight: The Role Of Sleep
Poor sleep increases inflammation and slows barrier repair. Even one night of bad sleep can make your gut and skin more leaky.
This means that improving sleep is one of the simplest ways to support your barriers. People who work night shifts or have irregular sleep often have more gut and skin problems.
Non-obvious Insight: Microbiome Imbalance
Your microbiome (good bacteria living in your gut and on your skin) helps keep barriers strong. If you lose these friendly bacteria (after antibiotics, for example), your barriers become weaker and inflammation rises.
Some skin conditions, like acne or eczema, are linked to changes in skin bacteria. The same happens in the gut—less diversity in bacteria means weaker barriers and more inflammation.
Practical Ways To Break The Cycle
Breaking the inflammation-barrier cycle takes time and a smart strategy. Here are proven ways to help:
1. Eat Barrier-friendly Foods
Choose foods that lower inflammation and support your barriers, such as:
- Fiber-rich foods: Oats, beans, fruits, and vegetables feed good gut bacteria.
- Healthy fats: Olive oil, avocados, and nuts help build strong cell walls.
- Fermented foods: Yogurt, kefir, and sauerkraut add good bacteria.
- Omega-3s: Found in fish, flaxseed, and walnuts. They lower inflammation.
Eat a wide variety of plants to get different fibers. The more types of fiber you eat, the more types of good bacteria you support. Try adding new vegetables or fruits each week.
Avoid:
- High sugar and processed foods
- Artificial additives
- Too much alcohol
Processed foods often contain emulsifiers or preservatives that harm gut bacteria and barriers. Even “healthy” snacks can sometimes have these additives, so read labels.
2. Protect Your Skin
- Use mild, fragrance-free cleansers.
- Moisturize after washing.
- Avoid hot showers.
- Wear gloves when using chemicals.
Simple habits, like patting your skin dry instead of rubbing, can help keep the barrier intact. Moisturizing within minutes after washing locks in water and strengthens the skin.
3. Manage Stress
Chronic stress increases inflammation. Try:
- Deep breathing or meditation
- Gentle exercise like walking or yoga
- Good sleep habits
Stress hormones, like cortisol, make barriers more leaky. Taking breaks, practicing gratitude, or spending time in nature can all help lower stress.
4. Support Your Microbiome
- Avoid unnecessary antibiotics.
- Take probiotics if your doctor suggests.
- Eat prebiotic foods (onion, garlic, banana).
Prebiotics are special fibers that feed good bacteria. Try to include them daily, as they work best when eaten often, not just once in a while.
5. Get Enough Sleep
Aim for 7-9 hours each night. Sleep helps your body repair damage and keeps inflammation down.
Set a regular bedtime, keep screens out of the bedroom, and avoid caffeine late in the day. These small changes can have a big impact on your barriers and immune system.
6. Avoid Unnecessary Medications
Some medicines can hurt your barriers. Always ask your doctor if you really need them.
Non-steroidal anti-inflammatory drugs (NSAIDs), for example, can harm the gut lining if used too often. Always follow your doctor’s advice and do not stop needed medicines without talking to them.
7. Stay Active
Regular exercise lowers inflammation and supports healthy barriers.
You don’t need intense workouts—walking, cycling, or swimming all help. Exercise also improves sleep and reduces stress, creating a positive loop.
8. Avoid Toxins And Allergens
- Use air filters at home
- Don’t smoke
- Limit exposure to strong chemicals
If you live in a polluted area, keeping windows closed on high pollution days and using indoor plants can also help reduce exposure.
9. Treat Infections Quickly
See a doctor if you have a fever, wound, or ongoing cough. Early treatment prevents long-term inflammation.
Ignoring infections can turn a small problem into chronic inflammation. Keep wounds clean and follow up if you do not heal as expected.
10. Consider Supplements
Some people benefit from vitamin D, zinc, or omega-3 supplements. Ask your doctor before starting.
Supplements are not magic bullets but can help if you have a deficiency. Blood tests can show if you need extra support.
The Science: Data And Studies
Scientists have found strong links between inflammation, barrier damage, and disease.
- In one study, people with inflammatory bowel disease had 10 times more leaks in their gut lining compared to healthy people.
- Children with eczema are 2-3 times more likely to develop asthma or allergies because their broken skin lets in more triggers.
- People who sleep less than 6 hours a night have higher levels of C-reactive protein (CRP), a marker of inflammation.
- Eating fiber-rich diets can lower inflammation by 29% and improve gut barrier strength.
Another study found that children who grew up with a pet dog or on a farm had stronger gut barriers and fewer allergies. This shows that early exposure to healthy bacteria helps barriers develop properly.
Comparing Barriers And Their Risks
Here is a comparison of different barriers, what damages them, and diseases linked to their breakdown:
| Barrier | Main Damage Triggers | Diseases Linked |
|---|---|---|
| Skin | Allergens, harsh soaps, dry air | Eczema, infections |
| Gut lining | Poor diet, stress, antibiotics | IBD, food allergies, autoimmune |
| Lung lining | Pollution, smoke, viruses | Asthma, bronchitis |
| Blood-brain barrier | Inflammation, infections | MS, Alzheimer’s, brain fog |
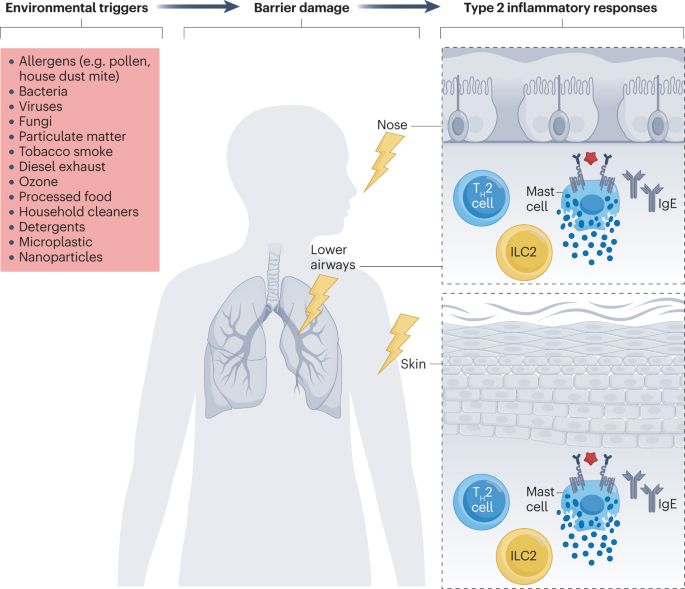
Credit: www.nature.com
Signs Your Barrier Is Damaged
You may not notice barrier damage right away, but watch for these warning signs:
- Chronic diarrhea, bloating, or stomach pain
- Frequent skin rashes or infections
- Asthma or chronic cough
- Brain fog, trouble thinking clearly
- Fatigue that doesn’t improve with rest
- Food or chemical sensitivities
Some people also notice slow wound healing, brittle nails, or hair thinning as signs of poor barrier health. If you see these changes, consider your lifestyle and talk to a doctor.
If you have these symptoms often, talk to your doctor.
The Role Of The Microbiome
Your microbiome is a community of trillions of bacteria, viruses, and fungi that live in your gut, on your skin, and in your mouth. These tiny creatures are essential for strong barriers and low inflammation.
How The Microbiome Protects You
- Competes with harmful germs for space
- Produces short-chain fatty acids (SCFAs) that feed gut cells
- Signals the immune system to calm down
SCFAs are like food for your barrier cells. Without enough, the cells get weak, and gaps appear in the wall. That’s why diets high in fiber and fermented foods are so helpful.
When your microbiome is diverse and healthy, your barriers stay strong. But:
- Antibiotics, poor diet, or stress can reduce good bacteria.
- This makes barriers weaker and raises inflammation.
A diverse microbiome is like a rich garden—it keeps weeds (bad bacteria) out and helps the soil (your body) stay healthy.
Comparing Foods For A Healthy Microbiome
Here’s a look at foods that support or harm your microbiome:
| Helpful Foods | Harmful Foods |
|---|---|
| Yogurt, kefir, kimchi | Soda, candy, chips |
| Beans, oats, bananas | Processed meats, fried foods |
| Leafy greens, garlic, onions | Artificial sweeteners |
Try to include helpful foods every day. Changing your microbiome can take weeks or months, but the benefits grow over time.
Chronic Diseases Linked To The Cycle
Many chronic diseases start with barrier damage and ongoing inflammation. Some common examples:
- Irritable Bowel Syndrome (IBS): Leaky gut triggers pain, bloating, and diarrhea.
- Eczema: Broken skin barrier leads to rashes and infections.
- Asthma: Damaged lung lining lets in allergens, causing wheezing.
- Type 1 Diabetes: Immune cells attack pancreas after gut barrier leaks.
- Multiple Sclerosis (MS): Immune cells cross a leaky blood-brain barrier and attack nerves.
Data Snapshot
- Up to 70% of people with food allergies have a leaky gut.
- Over 90% of people with eczema have a weak skin barrier.
- Asthma rates are 2-3 times higher in cities with more air pollution due to lung barrier damage.
Many autoimmune diseases, like rheumatoid arthritis or lupus, also start with barrier problems. When the body’s own barriers are damaged, the immune system can get confused and attack healthy cells.
How Doctors Diagnose Barrier Damage
Doctors use several tests to check for barrier damage and inflammation:
- Blood tests for CRP, white blood cell count, or antibodies
- Stool tests for gut inflammation or leaky gut markers (like zonulin)
- Skin patch tests for allergies and barrier weakness
- Lung function tests for asthma and bronchitis
- Imaging (like MRI) for blood-brain barrier issues
Early diagnosis helps you break the cycle before it causes more problems.
Doctors may also ask about your diet, stress, and family history to find possible triggers. Keeping a health diary can help spot patterns in symptoms.
Real-world Example: Breaking The Cycle
Let’s look at a case:
Maria, age 32, had eczema and stomach issues for years. She often ate processed foods, slept poorly, and was under stress. Her doctor found signs of leaky gut and weak skin barrier.
What worked for Maria:
- She switched to a fiber-rich, low-sugar diet.
- She used mild skin products.
- She practiced daily meditation.
- She took a probiotic supplement.
After 6 months, her skin improved, digestion was better, and she had more energy. This shows that small changes can break the inflammation-barrier cycle.
Maria’s story is common. Many people see better results with simple, steady changes than with drastic diets or extreme routines. Patience and consistency are key.
Key Takeaways For Breaking The Cycle
To keep your barriers strong and inflammation low:
- Eat a healthy, fiber-rich diet.
- Protect your skin and lungs from harsh chemicals.
- Get regular exercise and enough sleep.
- Manage stress with relaxation techniques.
- Take care of your microbiome.
- Avoid unnecessary antibiotics and medications.
- Treat infections early.
- Watch for warning signs and talk to your doctor.
Remember, you do not have to do everything at once. Start with one change, build a habit, and add more steps as you feel ready. Over time, your body will thank you.

Credit: harlanmd.com
Common Mistakes To Avoid
Even with good intentions, some mistakes can keep the cycle going:
- Using harsh soaps or alcohol-based sanitizers too often
- Skipping meals or eating lots of processed snacks
- Ignoring stress or not getting enough sleep
- Overusing antibiotics or painkillers
- Not finishing prescribed treatments for infections
Some people also make the mistake of stopping their new habits once they feel better. It’s important to keep up with healthy routines, even after symptoms improve, to prevent the cycle from starting again.
Breaking the cycle is not about perfection. It’s about making steady, smart choices.
Data: Barrier Health And Lifestyle Choices
Research shows that lifestyle changes can lower inflammation and repair barriers. For example:
- People who switch to a Mediterranean diet (high in fruits, vegetables, and healthy fats) have 30% lower inflammation markers.
- Regular exercise (150 minutes a week) improves gut barrier function and lowers asthma risk by up to 40%.
- Quitting smoking restores lung lining strength within 6 months.
Even small improvements, like adding one serving of vegetables a day or walking after meals, can help. The benefits add up over time.
Table: Impact Of Lifestyle Habits On Barriers
| Lifestyle Habit | Effect on Barriers | Effect on Inflammation |
|---|---|---|
| High fiber diet | Strengthens gut lining | Reduces inflammation |
| Regular exercise | Protects lung and gut | Lowers CRP levels |
| Good sleep | Supports repair | Reduces stress hormones |
| Smoking | Damages lung lining | Raises inflammation |
| Processed foods | Weakens gut barrier | Raises inflammation |
When To See A Doctor
If you keep having symptoms like rashes, stomach pain, or coughs, see your doctor. They can test for barrier damage and help you create a plan. Do not ignore ongoing signs, especially if you have a family history of chronic diseases.
Doctors can also help guide you on which changes are most important for your health. Don’t wait until symptoms are severe—early action is best.
Future Research: Can We Fully Restore Barriers?
Scientists are testing new ways to repair barriers:
- Special probiotics and prebiotics to grow good bacteria
- Drugs that block harmful immune chemicals
- Stem cell treatments to rebuild barriers
- Personalized diets based on your genes and microbiome
One exciting study found that giving mice a certain gut bacteria repaired leaky gut and stopped autoimmune disease. While human treatments are still in early stages, the future looks hopeful.
There is also research into using topical creams with special fats for eczema, or inhaled treatments for asthma, to directly strengthen barriers. The goal is to find targeted therapies with fewer side effects.
If you want to learn more about the science behind inflammation and barrier health, visit this research paper for deeper details.
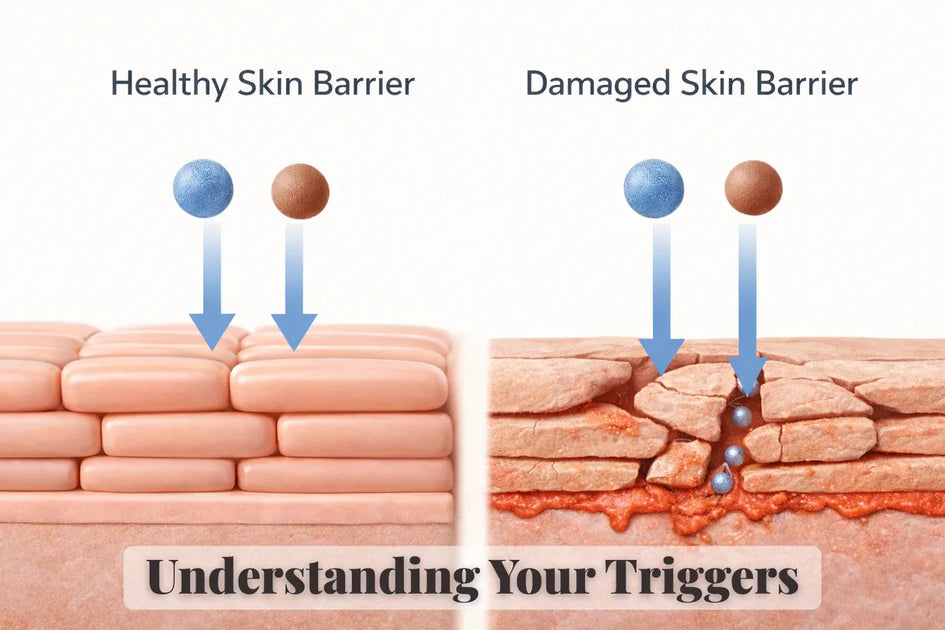
Credit: harlanmd.com
Frequently Asked Questions
What Is The Main Cause Of Barrier Damage?
The most common causes are chronic inflammation, poor diet, stress, infections, and harsh chemicals. These break down the tight walls of your skin, gut, or lungs.
How Do I Know If My Gut Barrier Is Damaged?
Signs include bloating, diarrhea, food sensitivities, and brain fog. Doctors can check with blood or stool tests for markers like zonulin.
Can Supplements Help Repair Barriers?
Some supplements, like probiotics, vitamin D, and omega-3s, may help, but they work best with a healthy diet and lifestyle. Always check with your doctor first.
Is All Inflammation Bad?
No. Acute inflammation helps your body heal. But chronic inflammation can cause barrier damage and disease if it does not stop at the right time.
Can The Cycle Be Fully Reversed?
In many cases, yes. With the right food, habits, and medical care, barriers can heal, and inflammation goes down. Some diseases may need longer treatment, but improvement is possible for most people.
Inflammation and barrier damage are deeply connected, but you have the power to break the cycle. Start with small changes, listen to your body, and get help when needed. Your health is worth it.
