Perioral dermatitis is a skin problem that often brings frustration, discomfort, and confusion. It shows up as small red bumps, flakiness, and irritation around the mouth and sometimes the eyes or nose. Many people try different creams and treatments, but often, the skin barrier is left damaged and weak. This is why barrier repair is so important. If you understand how to rebuild your skin’s natural defense, you can calm symptoms and get your skin healthy again. In this guide, you will learn a gentle, step-by-step protocol for barrier repair in perioral dermatitis. You will also find practical tips, common mistakes to avoid, and answers to frequent questions.
Understanding Perioral Dermatitis And The Skin Barrier
Perioral dermatitis is a facial rash that looks similar to acne or eczema but has its own causes and treatments. It appears as clusters of red bumps, sometimes with pus, surrounded by dry, flaky, or sensitive skin. The exact cause is not always clear, but there are common triggers:
- Topical steroids (even over-the-counter hydrocortisone)
- Heavy skin creams or ointments
- Fluorinated toothpaste
- Hormonal changes
- Harsh or overused skincare products
It’s important to understand that perioral dermatitis is not an allergy or an infection in most cases. Instead, it’s often a reaction to something that weakens your skin’s natural defense system. Even people who have never had skin problems before can develop this rash if their barrier gets damaged.
The skin barrier is a thin layer on the surface that keeps moisture in and harmful things out. This barrier is made up of skin cells held together by lipids—mainly ceramides, cholesterol, and fatty acids. Think of it like a brick wall: the cells are bricks, and the lipids are the mortar. When this barrier is damaged, your skin loses water, becomes dry, and lets irritants in more easily. In perioral dermatitis, repairing the barrier is just as important as calming the rash. Without a strong barrier, the problem often comes back.
One insight many people miss is that even “gentle” products can be too harsh for compromised skin. For example, some cleansers labeled as mild still contain surfactants that strip away oils. Also, environmental factors—like dry air or wind—can further weaken the barrier without you realizing it.
Why Barrier Repair Is Essential
Many treatments for perioral dermatitis focus on stopping inflammation or fighting bacteria. But if you only use antibiotics or anti-inflammatories, you miss a key part: helping the skin to heal itself. A broken barrier lets triggers keep causing trouble. When you focus on barrier repair, you help your skin:
- Hold onto moisture better
- Resist new irritants
- Heal faster and more completely
A strong barrier also makes other treatments work better and reduces your risk of long-term redness or sensitivity. This is because healthy skin can “bounce back” from stress or minor irritants, while a damaged barrier means even small triggers can cause big reactions.
Another detail many overlook: when your barrier is healthy, your skin is less likely to develop new allergies or sensitivities. Damaged skin allows more allergens to penetrate, sometimes causing issues that never existed before. So, barrier repair isn’t just about healing today—it’s also about protecting your skin for the future.
The Gentle Rebuild Protocol: Step-by-step
Healing perioral dermatitis requires patience. The gentle rebuild protocol is about using the right products, in the right way, and avoiding common mistakes. Each step supports your skin’s natural healing.
Step 1: Simplify Your Routine
The first step is to stop using anything that might be making things worse. That means cutting out:
- Steroid creams (unless your doctor insists)
- Heavy moisturizers, especially those with petrolatum or mineral oil
- Fragranced skincare or toothpaste
- Physical or chemical exfoliants
- Multiple-step routines with many actives
Many people feel the urge to use more products when their skin is not improving. But extra steps usually slow down recovery. “Less is more” is especially true for perioral dermatitis.
Instead, focus on a minimal routine:
- Gentle cleanser (no sulfates, no scrubs)
- Simple, soothing moisturizer
- Sun protection (mineral sunscreen is usually best)
Sometimes, stopping all products for a few days—called a “product holiday”—can give your skin a reset. However, do not leave skin dry for too long; always restart a basic moisturizer as soon as possible.
Step 2: Choose The Right Cleanser
Cleansing is important, but too much can damage your barrier. Choose a very mild cleanser. Look for these features:
- No sulfates (SLS or SLES)
- Fragrance-free
- Creamy or lotion texture, not foaming
- PH balanced (between 5.0 and 5.5)
Example: You can use a micellar water or a non-foaming cleanser once a day, at night. In the morning, rinsing with water is often enough.
Be sure to avoid washcloths, brushes, or sponges. Even soft tools can irritate delicate skin. Your fingertips are the best tool for cleansing.
Many people believe that “clean skin is healthy skin,” but over-cleansing actually makes things worse. If your skin feels tight or squeaky after washing, your cleanser is too harsh. A good test: your face should feel comfortable and soft after washing, not dry.
Step 3: Moisturize With Purpose
Moisturizing is key for rebuilding the barrier, but you need the right kind of moisturizer. The best ones for perioral dermatitis have:
- Ceramides: Help rebuild the natural barrier
- Glycerin or hyaluronic acid: Pull water into the skin
- Fatty acids: Strengthen and soften the skin
- No perfumes, essential oils, or heavy oils
Apply a small amount after cleansing, while the skin is still slightly damp. Don’t rub or massage hard—just gently pat it in.
If your skin stings when you apply moisturizer, try using a “sandwich” method: rinse with water, apply a thin layer of moisturizer, wait a few minutes, then add another thin layer. This can reduce stinging and help the product absorb better.
Remember, you may need to adjust the amount you use based on weather or how your skin feels. In dry or cold climates, a thicker layer might help; in humid weather, less is more.
Step 4: Use Mineral Sunscreen
Sun can make perioral dermatitis worse. But many sunscreens irritate sensitive skin. Choose a mineral sunscreen with zinc oxide or titanium dioxide. These are less likely to sting or clog pores. Look for:
- SPF 30 or higher
- No added fragrance or alcohol
- Cream or lotion texture
Apply sunscreen every morning, even on cloudy days. Reapply if you’re outside for long periods.
Some people skip sunscreen because they fear it will make the rash worse. The key is to patch test first and start with a small amount. If you are indoors most of the day, you can apply sunscreen only to exposed areas, but always use it if you’ll be near windows or outside.
Step 5: Avoid Triggers Completely
Some triggers are easy to miss. For example, even “natural” toothpaste can have irritating oils. Pay special attention to:
- Toothpaste: Use one without fluoride, SLS, or strong flavor oils
- Lip balms: Avoid menthol, camphor, or fragrance
- Hair products: Keep them away from your face
- Pillows and towels: Wash often, use gentle detergent
If you’re not sure about a product, try a patch test on your inner arm for a few days first.
Another often-missed trigger is hand-to-face contact. If you rest your chin in your hands or touch your face during the day, oils and bacteria can transfer to sensitive areas. Being mindful of this small habit can reduce flares.
Step 6: Support Your Skin From The Inside
Healthy skin depends on your whole body. Focus on:
- Drinking enough water
- Eating foods rich in omega-3 fatty acids (like salmon, walnuts, flaxseed)
- Avoiding high-sugar and processed foods
- Managing stress (which can make skin flare up)
These steps help your skin heal faster and reduce the chance of a return.
A non-obvious tip: address gut health. Digestive problems can sometimes show up as skin problems. Eating more fermented foods (like yogurt or sauerkraut) may help balance gut bacteria, which can support your skin’s healing.
Step 7: Add Barrier-repair Boosters (if Needed)
If your skin is very dry, you can add a barrier-repair booster. These are serums or creams with extra ceramides, cholesterol, or fatty acids. Use a small amount, once a day, and only after patch testing.
A few well-known options:
- Ceramide serums
- Cholesterol-rich creams
- Squalane oil (if tolerated; use sparingly)
Remember, more is not always better. If something stings or worsens redness, stop and go back to basics.
Also, introduce only one booster at a time. If you add multiple new products at once, you won’t know which one is causing a reaction if your skin gets worse.
Step 8: Be Patient And Consistent
Barrier repair is slow. It can take weeks or even months for full healing. Do not expect instant results. Signs your barrier is improving include:
- Less dryness and flaking
- Redness fades
- Bumps reduce in number
- Skin feels more comfortable
Stick with the simple routine, and resist the urge to try new products too soon.
For faster improvement, keep a daily skin journal. Write down what you use, how your skin feels, and any changes. This can help you spot patterns and avoid repeating mistakes.
How To Choose Barrier-repair Products
Not all “barrier repair” products are truly helpful. Some contain hidden irritants or too many ingredients. Here’s what to look for when you shop.
Key Ingredients For Barrier Repair
The most helpful barrier-repair ingredients are:
- Ceramides: These are natural fats found in your skin. They help seal in moisture and protect against irritants.
- Glycerin: Attracts water from the air into your skin, keeping it hydrated.
- Hyaluronic acid: Holds water in your skin, making it plump and less flaky.
- Squalane: A gentle, skin-identical oil that helps prevent water loss.
- Cholesterol: Works with ceramides to build a strong barrier.
- Fatty acids: Like linoleic acid, help repair and soften skin.
A little-known fact: products with all three—ceramides, cholesterol, and fatty acids—work better than products with just one or two. This combination closely matches your skin’s natural “mortar.”
Ingredients To Avoid
Avoid products with:
- Fragrance or essential oils: These can irritate sensitive skin
- Alcohol (denatured or SD): Dries out the skin
- Harsh actives: Like retinoids, vitamin C, benzoyl peroxide, or exfoliating acids
- Silicones: Sometimes fine, but can trap heat if skin is inflamed
One hidden source of irritation: preservatives like methylisothiazolinone or parabens can sometimes bother very sensitive skin. If you notice burning or stinging, check for these in the ingredient list.
Product Texture And Packaging
Creams are usually better than lotions for barrier repair, because they have more oils and moisture. Tubes or pumps are safer than jars (less chance of bacteria).
A tip: If you need to use a jar, always scoop product out with clean hands or a spatula, not your fingers.
Comparing Moisturizer Ingredients
Here is a quick look at how common moisturizers differ in their key ingredients:
| Product Name | Ceramides | Glycerin | Fragrance-Free | Texture |
|---|---|---|---|---|
| CeraVe Moisturizing Cream | Yes | Yes | Yes | Cream |
| Vanicream Moisturizing Cream | No | Yes | Yes | Cream |
| La Roche-Posay Lipikar Balm AP+ | Yes | Yes | Yes | Thick Balm |
| Avene Tolerance Control | No | Yes | Yes | Light Cream |
Choose a product that fits your skin’s needs—very dry skin may need a thicker balm, while oily skin might prefer a lighter cream. Another tip: switching between creams seasonally can help. Use thicker formulas in winter and lighter ones in summer.

Credit: harlanmd.com
What To Expect During Healing
It’s normal to feel impatient when your skin is red, flaky, or bumpy. Knowing what to expect can help you stick with the protocol.
Timeline Of Barrier Repair
- First few days: Redness may not change much. You may even see some flaking as old skin sheds.
- 1-2 weeks: Bumps begin to shrink. Skin feels less tight or itchy. Less new irritation.
- 1 month: The barrier is stronger. Fewer flare-ups. Moisture stays in the skin better.
- 2-3 months: Skin looks more even, less sensitive, and feels “normal.”
Healing can also be affected by things outside your control, such as hormonal changes or weather. If your progress stalls, look for new triggers or discuss changes with your doctor.
Some people heal faster, especially if they haven’t used steroid creams for long. Others may need more time. If the rash gets worse, or you see pus, pain, or spreading, see a dermatologist.
Common Healing Signs
- Flaking or peeling (as old, damaged skin comes off)
- Temporary pinkness
- Slight itch as skin renews
These are normal unless they are severe or painful.
It’s also common for skin to look worse before it gets better. This is called “transitional flaring” and usually passes in a few days.
When To Worry
If you experience:
- Sudden swelling
- Spreading redness or pus
- Pain or burning
- No improvement after 2 months
Get professional advice. Sometimes, prescription antibiotics or other treatments are needed.
Mistakes To Avoid In Barrier Repair
Many people make the same errors that slow down healing or cause setbacks. Here are the most common mistakes and how to avoid them.
- Doing too much, too soon: Adding new products, masks, or treatments every few days can irritate skin and undo progress.
- Using hot water: Hot water strips natural oils and can worsen dryness. Use lukewarm water only.
- Scrubbing or picking: Trying to remove flakes or bumps can lead to infection or scarring.
- Re-starting steroids: Using steroid creams for quick relief usually leads to a rebound—stronger rash when you stop.
- Ignoring triggers: Not switching toothpaste or continuing to use fragranced products keeps the cycle going.
- Not patch testing: Even barrier creams can irritate some people. Test on a small area first.
- Skipping sunscreen: Sun damage makes the barrier weaker, even if you don’t burn.
- Changing routines too quickly: Allow at least 2-3 weeks before judging if something is working.
A less obvious mistake is not washing your hands before applying products. This can transfer bacteria and dirt, making healing slower.
Comparing Barrier-repair Protocols
Different sources suggest different approaches. Here’s a look at how the gentle rebuild protocol compares to a more aggressive, medication-first protocol.
| Approach | Focus | Speed | Risk of Flare-Ups | Side Effects |
|---|---|---|---|---|
| Gentle Rebuild Protocol | Barrier repair, trigger avoidance | Slower (weeks to months) | Lower (if patient) | Minimal |
| Medication-First Protocol | Topical/oral antibiotics | Faster (days to weeks) | Higher (if barrier not repaired) | Possible irritation, dryness |
The gentle approach is better for long-term health, especially if you want to avoid antibiotics. Even if you need medication, combining it with barrier repair gives the best results and prevents future flares.
Practical Tips For Everyday Life
Barrier repair is not just about products—it’s about habits and routines. Here are practical tips to support healing every day.
- Wash hands before touching your face. This prevents bacteria and dirt from causing new irritation.
- Change pillowcases often. Oils and bacteria build up quickly. Use gentle, fragrance-free laundry detergent.
- Avoid face masks with harsh ingredients. Clay, acids, or charcoal can strip your skin’s barrier.
- Wear a scarf or face shield in cold, windy weather. Wind and cold can dry out skin quickly.
- Shave carefully. Use a fragrance-free, gentle shaving cream, and avoid shaving too often.
- Limit makeup use. If you must use makeup, choose mineral formulas and remove gently at night.
If you live in a dry climate, consider using a humidifier in your bedroom. This adds moisture to the air, which helps your skin heal.
For those who exercise, sweat can sometimes cause irritation. Rinse your face with cool water after workouts, and reapply moisturizer if needed.
How Diet And Lifestyle Can Help
Good skin starts from inside. While perioral dermatitis is not always caused by diet, certain foods and habits can speed up healing.
Best Foods For Barrier Repair
- Fatty fish (salmon, sardines): Rich in omega-3s that reduce inflammation
- Seeds and nuts (flaxseed, walnuts): Plant sources of healthy fats
- Colorful vegetables: Provide vitamins A, C, and E, which help skin renew
- Water: Staying hydrated helps skin heal faster
A less obvious support: zinc-rich foods (like beans, pumpkin seeds, and whole grains) can help the skin repair itself, especially if your diet is low in zinc.
Foods And Habits To Avoid
- Sugary snacks and drinks: Sugar can cause more inflammation
- Spicy foods: Sometimes trigger flares in sensitive people
- Alcohol: Dries out the skin and makes healing slower
- Smoking: Damages blood flow to the skin
If you’re unsure whether a food is a trigger, try keeping a food diary. Write down what you eat and how your skin reacts. Over time, you may spot a pattern.
Stress Management
Stress can trigger or worsen perioral dermatitis. Try:
- Gentle exercise (walking, yoga)
- Mindfulness or meditation
- Getting enough sleep
If you feel stress is a major factor, speaking with a counselor or therapist can help you manage stress better—and support your skin’s healing.
When To See A Dermatologist
Most mild cases of perioral dermatitis improve with gentle barrier repair and careful trigger avoidance. But sometimes you need expert help. Seek professional advice if:
- The rash spreads or gets painful
- You see yellow crusts, pus, or swelling
- No improvement after 2-3 months
- You are unsure about what products to use
A dermatologist can prescribe topical or oral antibiotics, or check for other skin problems. Sometimes, a skin scraping or culture is needed to rule out infection.
Remember, perioral dermatitis is a medical condition. If you have any doubt, it’s always better to ask an expert rather than try to fix it alone.
Children And Perioral Dermatitis
Children can also get perioral dermatitis, especially if they use topical steroids or toothpaste with SLS. The same gentle approach works for most kids, but always check with a doctor before using new creams or treatments.
- Use a mild, fragrance-free moisturizer
- Stop all steroid creams unless prescribed
- Switch to gentle toothpaste
- Protect skin from the sun
Children’s skin heals quickly, but barrier repair is still important for long-term skin health.
One tip: remind children not to lick around their mouths, as saliva can dry and irritate the skin further.

Credit: harlanmd.com
The Role Of The Microbiome
Recent research shows that the skin microbiome—the balance of good and bad bacteria on your skin—plays a role in perioral dermatitis. Overusing harsh cleansers, steroids, or antibiotics can upset this balance. Supporting your barrier also helps healthy bacteria return.
- Use gentle, microbiome-friendly skincare
- Avoid unnecessary antibiotics or antiseptics
- Consider probiotic-rich foods (yogurt, kefir)
A healthy microbiome may reduce flares and speed up healing.
For example, some new moisturizers include “prebiotics” or “probiotics” designed to feed good bacteria. While research is still early, these may offer extra help for sensitive skin.
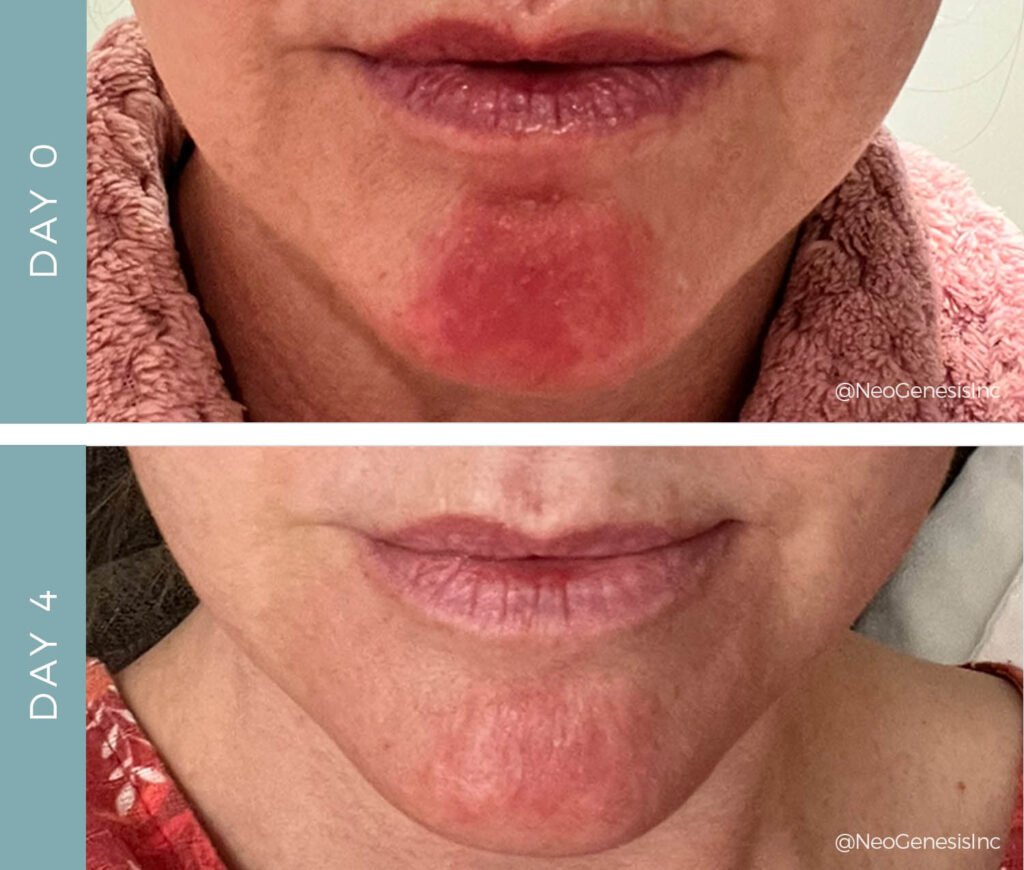
Real-life Examples
Many people have healed perioral dermatitis with the gentle rebuild protocol. Here are two real-world cases:
- Anna, age 32: Developed red bumps around her mouth after using a steroid cream for eczema. She stopped the steroid, switched to a ceramide-rich moisturizer and non-foaming cleanser, and saw slow but steady improvement over two months. She avoided toothpaste with SLS and heavy makeup. Her skin is now clear and less sensitive.
- Sam, age 25: Tried antibiotic creams for months with little improvement. After switching to a simple routine of gentle cleansing and moisturizing, plus using a mineral sunscreen, his rash faded within six weeks. He also cut out spicy foods and reduced stress with yoga.
A less obvious lesson from these cases: both Anna and Sam kept their routines simple. They did not add many new products at once, and they paid attention to small triggers, like toothpaste and stress.
Both examples show the power of patience, simplicity, and barrier repair.
Credit: neogenesis.com
Frequently Asked Questions
What Is The Fastest Way To Heal Perioral Dermatitis?
There is no instant cure, but the gentle rebuild protocol helps your skin heal naturally. Avoid triggers, use a simple routine, and protect your skin from the sun. In some cases, prescription antibiotics may be needed for fast relief, but this should be guided by a dermatologist. Quick fixes often lead to quick returns; slow, steady healing is more reliable.
Can I Use Makeup During Barrier Repair?
It’s best to avoid makeup until your skin is stronger. If you must use it, choose mineral-based powders (not creams or liquids) and remove it gently with a mild cleanser. Do not use makeup with fragrance, essential oils, or alcohol. Wash makeup brushes often, and never share products with others.
Are Natural Oils Good For Perioral Dermatitis?
Some oils, like squalane, can help if used sparingly. Others, like coconut or olive oil, can clog pores or cause irritation. Always patch test first. Remember, not all “natural” products are gentle enough for damaged skin. Less is usually more when your skin barrier is weak.
How Long Does It Take For The Skin Barrier To Heal?
Most people see improvement in 2-6 weeks, but full barrier repair can take up to three months. Healing depends on stopping all triggers, using the right products, and being patient. If there is no progress after three months, see a dermatologist. Sometimes, hidden triggers or other skin conditions are involved.
Where Can I Find More Information About Skin Barrier Repair?
For more details on skin barrier function and repair, visit the American Academy of Dermatology. This site offers science-based advice on healthy skin routines.
Perioral dermatitis can be stubborn, but with the right approach, you can rebuild your skin’s barrier and enjoy comfortable, clear skin again. Be patient, gentle, and consistent—your skin will thank you.

