The relationship between how we feel inside and what shows up on our skin or hair is closer than many people think. You might notice that when you are stressed or anxious, your skin breaks out or your hair seems to fall more than usual.
Scientists and doctors have studied this connection for years. The truth is, our mental health and our skin and hair health are deeply linked. When something affects one, the other often responds.
But this connection is not just about feeling embarrassed when a pimple appears before an important event. Many skin and hair conditions are not only made worse by stress or mental health problems, but can also cause emotional struggles themselves.
This cycle can be hard to break, especially if you do not understand what is happening inside your body and mind.
This article will guide you through the science behind this connection, share real-life examples, and offer clear advice on how to care for both your mental health and your skin and hair. Whether you have acne, eczema, hair loss, or just want to understand yourself better, you will find helpful and trustworthy information here.
How Mental Health Affects Skin
Many people notice changes in their skin during stressful or emotional times. But why does this happen? The answer lies in our body’s response to stress and emotions.
The Mind-skin Connection
Your skin is the largest organ in your body and has thousands of nerves connected to your brain. When you feel stress or strong emotions, your body releases hormones like cortisol (the stress hormone). High levels of cortisol can:
- Increase oil (sebum) production in skin, leading to acne
- Make the skin barrier weaker, allowing irritants in and moisture out
- Slow down healing of wounds or skin damage
For example, one study found that students had more acne breakouts before exams, a time of high stress. Another report showed that people with chronic stress had drier, itchier skin compared to relaxed people.
Common Skin Conditions Linked To Mental Health
Some skin problems are especially sensitive to mental health:
- Acne: Stress makes acne worse by increasing oil and inflammation.
- Eczema (atopic dermatitis): Stress can trigger flare-ups or make itching worse.
- Psoriasis: Stress can cause new patches or worsen existing ones.
- Rosacea: Emotional changes can trigger redness and flare-ups.
- Hives: Anxiety can sometimes lead to sudden hives or rashes.
A study by the American Academy of Dermatology found that up to 40% of people with skin conditions also have symptoms of anxiety or depression.
Real-world Example
Consider someone preparing for a job interview. They may start to worry, leading to stress hormones rising. The next day, a pimple appears on their face, even if their skin was clear before. This makes them feel more anxious, creating a feedback loop that is hard to escape.
How Skin And Hair Conditions Affect Mental Health
It is not only that stress or anxiety can trigger skin and hair problems. The connection works in both directions. Many people with visible skin or hair issues feel embarrassed, sad, or anxious about how they look. This emotional effect can be very strong.
The Psychological Impact Of Skin Conditions
Having a skin condition like acne, eczema, or psoriasis can lower self-confidence and make social situations difficult. People may avoid going out, meeting friends, or even going to work or school because of their appearance.
In a survey, 70% of people with psoriasis said their condition affected their emotional well-being. Many reported feeling shame or embarrassment. Similar numbers are seen in people with acne and other skin problems.
Hair Loss And Mental Health
Hair is a big part of how we see ourselves. Losing hair, whether from stress, illness, or genetics, can have a big emotional impact.
- Alopecia areata (an autoimmune hair loss): Many people with this condition develop depression or anxiety.
- Telogen effluvium (stress-related hair loss): Sudden hair shedding often follows big life events or trauma.
A study in the Journal of the American Academy of Dermatology found that people with alopecia areata are twice as likely to have depression compared to those without the condition.
The Social Cycle
When someone feels bad about their skin or hair, they may avoid activities they enjoy. This isolation can worsen mental health, leading to more stress and, possibly, worse skin or hair. Breaking this cycle is important for both physical and emotional health.

Credit: www.rula.com
The Science Behind The Connection
Understanding how mental health and skin or hair conditions influence each other can help you manage both better.
The Brain-skin Axis
Doctors call the communication between your brain and skin the brain-skin axis. Signals travel from the brain to the skin through nerves, hormones, and the immune system. This is why emotions like fear, anger, or sadness can sometimes cause physical reactions like sweating, blushing, or itching.
Key Players
- Nerves: Carry messages from the brain to skin, affecting sweat glands, blood flow, and sensation.
- Hormones: Cortisol and other hormones travel in the blood and change how skin cells work.
- Immune System: Stress can change immune responses, making skin more likely to become inflamed or infected.
Biological Examples
When you are stressed, your body may:
- Release more histamine, leading to itching or hives
- Slow down skin healing by up to 40%
- Increase inflammation, making conditions like acne and psoriasis worse
The Role Of Inflammation
Chronic stress increases inflammation throughout the body. This inflammation can:
- Damage healthy skin cells
- Make existing skin conditions harder to treat
- Trigger new problems in people who did not have skin issues before
Skin Conditions Most Affected By Mental Health
Some skin problems are especially sensitive to mental health. Here is a closer look at some of the most common.
1. Acne
Acne is one of the most common skin conditions worldwide. Stress increases oil production and inflammation, two key causes of acne. Teenagers and adults both notice more breakouts during stressful periods. Even if you wash your face well, stress can still trigger pimples.
2. Eczema (atopic Dermatitis)
Eczema causes dry, itchy, inflamed skin. Stress can trigger flare-ups, make itching worse, and slow healing. People with eczema are more likely to report anxiety and sleep problems because of itching.
3. Psoriasis
Psoriasis is an autoimmune condition that leads to red, scaly patches. Stress does not cause psoriasis but often makes it worse. Flare-ups are common during times of emotional struggle.
4. Rosacea
Rosacea causes redness and visible blood vessels, especially on the face. Emotional changes like embarrassment, anger, or stress can trigger redness or burning.
5. Hives (urticaria)
Hives are raised, itchy welts that appear suddenly. They can be triggered by anxiety, stress, or even excitement.
6. Vitiligo
Vitiligo is a loss of skin pigment, leading to white patches. While the cause is not fully understood, stress is a known trigger for new patches.
7. Seborrheic Dermatitis
This condition causes flaky, oily, or red patches, often on the scalp or face. Stress can make it worse, possibly by changing oil production and immune responses.
8. Trichotillomania
This is a mental health disorder where a person pulls out their own hair, leading to bald patches. It is closely linked to anxiety and stress.
9. Dermatitis Artefacta
This rare condition involves self-inflicted skin damage, often as a way to cope with emotional pain.
Hair Conditions Linked To Mental Health
Just as with skin, hair problems can be both a cause and a result of mental health struggles.
1. Telogen Effluvium
This is sudden hair shedding, often after a stressful event, illness, or trauma. Hair follicles enter a resting phase and fall out a few months later.
2. Alopecia Areata
An autoimmune disorder where the immune system attacks hair follicles, causing patchy hair loss. Stress is a major trigger.
3. Trichotillomania
As mentioned earlier, this condition involves pulling out hair due to anxiety or stress.
4. Androgenetic Alopecia
Also called male or female pattern baldness, this is mostly genetic. However, emotional stress can speed up hair loss in some people.
5. Hair Graying
While genes play the biggest role, chronic stress may speed up graying in some people by damaging pigment cells.
The Vicious Cycle: When Skin, Hair, And Mind Affect Each Other
One of the hardest parts of having a skin or hair problem is the cycle it creates. Stress or anxiety can trigger a flare-up or hair loss. This makes you feel worse emotionally, leading to even more stress, which then makes your symptoms worse again.
For example, a person with eczema might have a flare-up during a stressful week. The red, itchy skin makes them feel embarrassed, leading to more stress and even worse skin.
Breaking this cycle usually requires treating both the physical symptoms and the emotional side at the same time.
Real Stories: Life With Skin And Hair Conditions
Many people live with skin or hair problems that affect their daily life and mental health. Here are a few real-world experiences:
- Maria, 21, with acne: “When my acne flares up before exams, I feel like everyone is staring at me. I skip parties and sometimes even classes. The more I worry, the worse my skin gets.”
- James, 35, with psoriasis: “My hands are always red and scaly. I feel embarrassed shaking hands at work. Stress at my job makes my skin worse, and it’s hard not to feel down.”
- Ananya, 28, with alopecia: “When I first lost a patch of hair, I was shocked and scared. I started wearing hats and avoiding mirrors. I felt anxious all the time and didn’t want to talk to anyone.”
These stories show that the emotional side of skin and hair conditions can be just as tough as the physical symptoms.
Data And Statistics: The Scope Of The Problem
The connection between mental health and skin or hair conditions is not just a few individual experiences. Research shows this is a global issue.
Here is a summary of some key data:
| Condition | % With Mental Health Impact | Common Emotional Effects |
|---|---|---|
| Acne | 50-70% | Anxiety, depression, low self-esteem |
| Psoriasis | 60-80% | Shame, embarrassment, isolation |
| Alopecia Areata | 40-60% | Depression, anxiety, social withdrawal |
| Eczema | 40-60% | Sleep problems, stress, anxiety |
In another survey, about 1 in 3 people with a skin condition said it affected their relationships and daily life.
The Role Of Childhood And Early Experiences
Early life stress can affect both mental health and skin or hair later in life. For example, children who experience trauma or ongoing stress are more likely to develop eczema or other skin issues as adults. This is because early stress can change how the immune system and stress response work.
Psychological Treatments That Help Skin And Hair
Treating skin or hair conditions is not just about creams or pills. Addressing the emotional side is important, too.
1. Cognitive Behavioral Therapy (cbt)
CBT is a type of talk therapy that helps people change negative thoughts and behaviors. Studies show CBT can reduce itching, anxiety, and depression in people with eczema, psoriasis, and other skin problems.
2. Stress Management
Relaxation techniques, mindfulness, and breathing exercises can lower stress hormones and improve skin health.
3. Support Groups
Meeting others with similar conditions can reduce feelings of isolation and offer practical tips for coping.
4. Psychiatric Medication
Sometimes, medication for depression or anxiety is helpful, especially if the emotional symptoms are severe.
5. Habit Reversal Therapy
For people with trichotillomania or skin picking, this therapy teaches new ways to manage urges.
| Therapy Type | Best For | Main Benefit |
|---|---|---|
| CBT | Acne, eczema, psoriasis | Reduces stress and negative thinking |
| Habit Reversal | Trichotillomania, skin picking | Breaks the cycle of self-harm |
| Support Groups | All chronic conditions | Emotional support, coping ideas |

Credit: www.emjreviews.com
Medical Treatments That Address Both Mind And Skin
Doctors sometimes use treatments that help both the skin and the mind.
- Antidepressants: Some antidepressants also reduce itching or help skin conditions.
- Antihistamines: Can reduce itching and help with sleep, improving mood and skin healing.
- Topical or oral steroids: Used for inflammation, but long-term use can affect mood and mental health.
It is important to talk with your doctor about how treatments affect both your skin and your emotions.
Lifestyle Tips To Improve Both Mental And Skin Health
Taking care of yourself inside and out can make a big difference.
1. Manage Stress
- Try meditation, yoga, or deep breathing
- Take breaks and rest when you feel overwhelmed
- Spend time outdoors or with loved ones
2. Sleep Well
Poor sleep increases stress hormones and can make skin problems worse. Aim for 7-9 hours per night.
3. Eat A Balanced Diet
Some studies suggest that diets high in sugar, dairy, or processed foods can make acne and other skin conditions worse. A diet rich in fruits, vegetables, lean proteins, and healthy fats supports both mental and skin health.
4. Avoid Skin Picking Or Hair Pulling
Try to notice when you feel the urge and use another activity (like squeezing a stress ball) instead.
5. Practice Gentle Skin Care
- Use mild cleansers and moisturizers
- Avoid harsh scrubs or strong chemicals
- Protect your skin from the sun
6. Reach Out For Help
If you feel overwhelmed, talk to a doctor, dermatologist, or mental health professional. Early support can break the cycle before it gets worse.
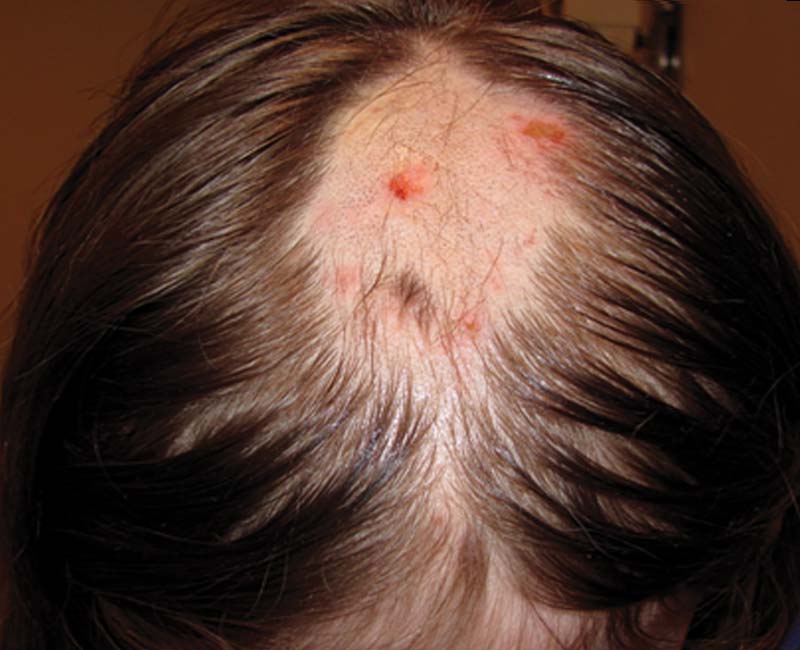
Credit: my.clevelandclinic.org
Myths About The Mind-skin-hair Connection
There are many myths about how mental health, skin, and hair are connected. Here are some facts:
- Myth: Only teenagers get acne from stress.
Fact: Adults can have stress-related acne, too.
- Myth: Skin problems are just “in your head.”
Fact: Skin conditions are real and have physical causes, even if stress is a trigger.
- Myth: If you just relax, your skin will be perfect.
Fact: Stress management helps, but many skin and hair conditions also need medical treatment.
When To See A Professional
If you notice any of these signs, it is a good idea to get help:
- Skin or hair problems are affecting your mood, sleep, or daily life
- You feel hopeless, depressed, or anxious most days
- You start to avoid people or activities because of your appearance
- You have thoughts of harming yourself
A professional can help you find the right treatment and support.
Non-obvious Insights Most People Miss
Many beginners focus only on creams or shampoos for their skin and hair. But here are two things most people do not realize:
- Chronic, low-level stress can be just as harmful to your skin and hair as big, sudden stress. Small worries that continue for weeks or months may slowly damage your skin barrier or hair growth.
- Social support is a powerful healer. People who have friends, family, or support groups cope better with skin and hair issues. Just talking about your struggles can lower stress and improve healing.
New Research And Future Directions
Scientists are learning more about the mind-skin-hair connection every year. Some exciting areas include:
- The role of the gut microbiome: New research suggests that the bacteria in your gut can affect both your mood and your skin. Eating foods that support gut health may help.
- Telemedicine: Online therapy and dermatology appointments are making it easier for people to get help, even if they feel embarrassed to go out.
- Personalized medicine: In the future, doctors may use your genetics and stress profile to choose the best treatment for you.
For more on this topic, see this detailed resource from the National Institutes of Health.
Frequently Asked Questions
What Is Psychodermatology?
Psychodermatology is the study of how the mind and skin affect each other. It combines dermatology (skin medicine) and psychology to treat both the skin and the emotional side of skin conditions.
Can Stress Really Cause Hair Loss?
Yes, high stress can cause types of hair loss like telogen effluvium or worsen other conditions like alopecia areata. Usually, hair grows back once stress is managed.
Are There Special Doctors For Skin And Mental Health?
Some dermatologists specialize in psychodermatology. Mental health professionals like psychologists or psychiatrists also help people cope with the emotional impact of skin or hair issues.
How Can I Tell If My Skin Or Hair Problem Is Linked To Stress?
If your symptoms get worse during stressful times, or you notice changes after big life events, stress may be a trigger. Keeping a diary of your symptoms and emotions can help spot patterns.
What Is The Best Way To Treat Both Skin/hair And Mental Health Together?
A combination approach works best: medical treatment for the skin or hair problem, plus stress management, therapy, and healthy lifestyle habits. Working with both a dermatologist and a mental health professional gives the best results.
Taking care of your mind, skin, and hair is not about vanity — it is about your total well-being. When you understand how these parts of you are linked, you can start breaking the cycle and feel better inside and out.
If you need help, reach out. Both your mind and your skin deserve care and respect.